We use cookies
We use cookies to ensure that we give you the best experience on our website. Would you like to accept all cookies for this site?
Nook Nik, Eyeworm (Thelaziasis)
Introduction
Nook Nik was a lactating female who presented to WVS Thailand's Rescue and Rehabilitation centre with left corneal ulceration and dehydration. The veterinary team diagnosed a worm, Thelazia spp, in both eyes. Systemic and topical treatment was initiated with a good response, and after an initial guarded prognosis for the left eye, Nook Nik made a good recovery with some permanent corneal scarring. This is her story.
History
Nook Nik was a 1 year old, 10 kg, lactating female dog with 4 puppies who were still nursing. She was presented to the WVS Thailand Rescue and Rehabilitation Centre with dehydration, dry skin, ocular discharge and left eye blepharospasm (excessive blinking of the eye). She had no history of vaccination or parasite prevention treatment.
Clinical Signs
Nook Nik was thin with a body condition score of 2/5. She had pale mucous membranes and her dehydration status was 7%. The skin across her back was mildly erythematous and dry with crusty patches of skin and all 4 limbs had patches of erythema.
Both eyes had normal palpebral and corneal reflexes. The right eye was clear but left eye was turbid and had a deep ulcer (Figure 1).
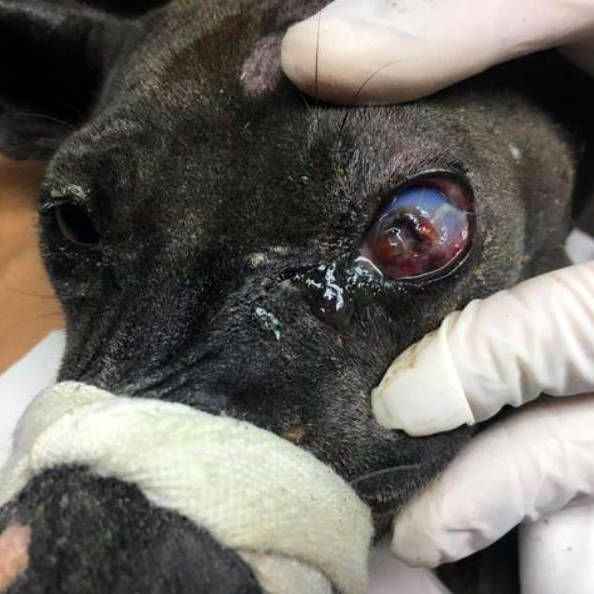
Figure 1 — Nook Nik’s eye at the time of presentation with severe corneal ulceration and ocular discharge.
The conjunctiva were inflamed and there was alopecia around both eyes. Both eyes had eyeworms under the eyelids and within the nictitating membrane and there was abundant seropurulent ocular discharge (Figure 2).
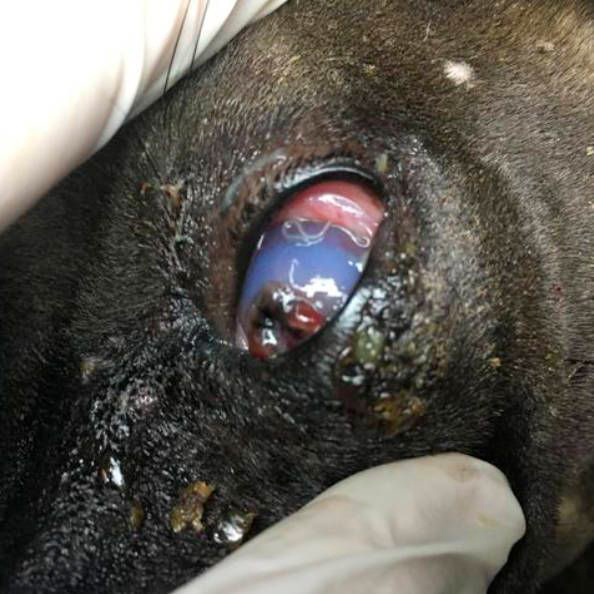
Figure 2 — The left eye with eyeworms visible under the eyelid, a central, corneal ulcer and seropurulent discharge.
Differential Diagnosis
Ocular
Due to the identification of eyeworms that were visible in both eyes, the top differential diagnosis was ocular thelaziosis caused by Thelazia callipaeda (species assumed based on geographical location), with secondary corneal ulceration, conjunctivitis, periocular alopecia, serous or purulent ocular discharge and corneal ulceration.
If we had not been able to identify the presence of eyeworms, differential diagnoses for corneal ulceration would be:
- Foreign Body
- Trauma
- Keratoconjunctivitis Sicca
- Eyelash or eyelid malformation e.g. entropion, ectopic cilia, large eyelid openings
- Neoplasia
- Facial or trigeminal nerve paralysis
Dermatology
Nook Nik's skin issues could be:
- Parasites e.g. mites, lice, fleas
- Bacterial
- Fungal
- Hypersensitivity
- Hypothyroidism
Diagnostic Work Up
Complete blood count and blood chemistry were performed to determine the patient’s general health status, together with a full physical examination.
The haematology results showed:
- Thrombocytosis (541,000 cells/cm³ [range 200,000-500,000 cells/³])
- Mild anaemia (Hct 32% [range 35-57%])
- Leukocytosis (21,500 cells/³ [range 6,000-17,000cells/³])
- Blood parasites not identified in the blood smear
A fluorescein stain was applied to the eye to assess the depth of the corneal ulceration. It showed complete and uninterrupted fluorescein staining of the ulcer, meaning that the ulcer was deep but had not quite gone as far as the Descemet's membrane (the last membrane of the cornea before the inner eye)
Skin scrapes of the lesions on her back and paws were negative for Demodex spp.
Treatment protocol
The first treatment phase involved manual removal of all Thelazia spp from the eye surface and under the eyelids and nictitating membrane. This involved a sterile saline flush, sterile cotton buds and forceps which were used to gently flush and remove the worms and carefully debride the corneal ulcer.
The initial plan was to try medical management of the corneal ulcer in the left eye; if this was not successful, enucleation would be carried out.
The eye was treated topically with antibiotic eye drops Poly-Oph® which contained a combination of neomycin sulphate, polymyxin B sulfate and gramicidin at a dose rate of 1 drop twice daily.
In addition, Nook Nik was treated systemically with:
- Ivermectin 600 µg/kg once per week injected subcutaneously
- Amoxicilin/clavulanic acid - 20mg/kg twice per day by mouth
- Tolfenamic Acid 4mg/kg subcutaneously at initial presentation
- Lactated Ringers solution, 200ml subcutaneously daily until rehydration was achieved
- FBC tablets (Vitamin B1, B2, B12 and C) once per day by mouth for 3 weeks
After 1 week of treatment, the corneal ulcer started filling up with scar tissue and Nook Nik's general condition was improving.
After 2 weeks, the lesion on her left eye was no longer positive for fluorescein stain indicating that the epithelial layer on the cornea had completely closed over. No further Thelazia spp had been found on clinical exam although Nook Nik's Schirmer Tear Test (a measure of the tear production capacity of the eye) was low. The course of artificial tears (Opsil tear) was therefore continued at 1 to 2 drops twice daily and as soon as she stopped feeding her puppies she was started on a course of prednisolone (Figure 3).

Figure 3 — Nook Nik’s eyes after treatment
Prognosis
The prognosis for thelaziosis largely depends on the lesions associated with the presence of the eyeworm. In Nook Nik's case, the deep corneal ulcer initially lead to a guarded prognosis (for the left eye) that was later changed to good after her positive response to the medical treatment.
Discussion
Thelazia spp (T. californiensis and T. callipaeda) are nematodes which infect the eyes of dogs, cats and other animals, including people. This parasite is commonly known as the “oriental eye worm” but is also found in Europe.
The first stage larvae (L1) localise under the third eyelid provoking lacrimation, conjunctivitis or even keratitis and corneal ulcer. L1s are released by the adult worms into the conjunctival secretions of infested animals and they are ingested by the flies which feed on these ocular secretions. Within the flies these L2’s develop into the infective third stage larvae (L3) within about 3 weeks.
The lifecycle of the eyeworm can be viewed here.The parasitic stage of Thelazia spp can be removed manually by rinsing with sterilised saline fluids or by collecting the adults with tweezers or a swab.
There are a few options for the use of antiparasitics for ocular thelazosis these include:
- Topical macrocyclic lactones e.g moxidectin
- Systemic macrocyclic lactone-containing products
- Spot-ons e.g Advocate®
- Oral formulations e.g Interceptor®, Milbemax®, Program Plus®, Sentinel®
Once the worms have been removed, treatment focuses on healing the damaged eye.
In this case, medical treatment was sufficient to heal Nook Nik’s corneal damage. The use of a broad spectrum antibiotic treatment was appropriate.
However, if Nook Nik had failed to respond to the medical treatment, or the damage was greater than in this case, the vet team could have performed a temporary tarsorrhaphy.
Tarsorrhaphy
Tarsorrhaphy is a procedure where the upper and lower eyelids are sewn together. This can be partial, at the medial or lateral aspects of the eye or complete.
The aim or tarsorrhaphy is to protect the corneal surface from exposure to further damage and to create an environment for the cornea to heal.
Horizontal mattress sutures are placed across both eyelids, ensuring that the sutures don’t enter into the ocular space and that they don’t cause the eyelids to roll inward. A space should be left at the medial canthus to allow administration of topical medications.
The sutures should stay in place for 2 weeks and they can either be removed sequentially or all at once, depending on the degree of damage and swelling. (Mohammad-Zadeh, 2011)
- CDC - DPDx - Thelaziasis. (2018, May 10).
https://www.cdc.gov/dpdx/thelaziasis/index.html
[Accessed 29 January 2019] - Mohammad-Zadeh, L. (2011). Treating Proptosis with Temporary Tarsorrhaphy.
https://www.atdove.org/article/treating-proptosis-with-temporary-tarsorr
[Accessed 17 March 2022] - Motta, B., Schnyder, M., Basano, F. S., Nägeli, F., Nägeli, C., Schiessl, B., Otranto, D. (2012). Therapeutic efficacy of milbemycin oxime/praziquantel oral formulation (Milbemax®) against Thelazia callipaeda in naturally infested dogs and cats. Parasites & Vectors, 5, 85.
https://doi.org/10.1186/1756-3305-5-85 - Otranto, D., Lia, R. P., Buono, V., Traversa, D., & Giangaspero, A. (2004). Biology of Thelazia callipaeda (Spirurida, Thelaziidae) eyeworms in naturally infected definitive hosts. Parasitology, 129(Pt 5), 627–633. Otranto, D., & Traversa, D. (2005). Thelazia eyeworm: an original endo- and ecto-parasitic nematode. Trends in Parasitology, 21(1), 1–4.
https://doi.org/10.1016/j.pt.2004.10.008 - Ruytoor, P., Déan, E., Pennant, O., Dorchies, P., Chermette, R., Otranto, D., & Guillot, J. (2010). Ocular Thelaziosis in Dogs, France. Emerging Infectious Diseases, 16(12), 1943–1945.
https://doi.org/10.3201/eid1612.100872

About the author
Dr. Anupat Tanseree (aka “Dr. Earth”) has been working with WVS Thailand since June 2018 after his graduation at Chiang Mai University (May 2018). Since then has been proved to be an enthusiastic and proactive young vet, quickly learning and proficiently training up to WVS protocols.
© WVS Academy 2026 - All rights reserved.